Are We Overestimating How Many Canadians Are Dying of COVID-19?
Viewpoint showing that without better information on the prevalence of the virus in the population, we risk overestimating COVID-19 deaths and mortality
Every day, Canadians are informed via press conference of the number of new deaths attributed to COVID-19. This publication by the Montreal Economic Institute raises questions about the accuracy of these statistics.
 Related Content
Related Content
 |
 |
 |
| Interview with Peter St. Onge (Danielle Smith, Global Radio, May 22, 2020) |
This Viewpoint was prepared by Peter St. Onge, Senior Fellow at the MEI, with the collaboration of Gaël Campan, Senior Economist at the MEI.
In late March 2020, NHS consultant Dr. John Lee worried that Britain would overestimate COVID-19 deaths and mortality in the absence of prevalence data.(1) Without better information on how many Canadians have been infected with COVID-19 and recovered, we risk making the same mistakes here in Canada.
As of May 5, known COVID-19 cases in Canada total 0.2% of the population.(2) However, a full month ago, the Angus Reid Institute released an epidemiological survey estimating that between 1% and 8% of Canadian households had already been infected by the virus.(3) April antibody studies from California similarly estimated that between 2.8% and 4.1% of the population had already been infected.(4) Given that Canada’s COVID-19 death rate is far higher than California’s,(5) we might expect Canada’s true prevalence to be somewhat higher than California’s.
Counterintuitively, higher prevalence is good news, because it suggests that the actual number of people dying from COVID-19 may be lower than we now estimate, while the disease itself may be far less lethal than we feared.
Estimating Comorbidity
This is because prevalence tells us how many people are dying “with COVID-19” as opposed to “from COVID-19.” To illustrate, if 95% of people have had a varicella infection (“chickenpox”)(6) at some point in their lives, the vast majority of deaths will have varicella antibodies. Of course, chickenpox is not killing those people; they are dying from comorbidities like cancer or heart disease. They died “with varicella” not “from varicella.”
As COVID-19 is far more fatal, we need to know what percent of people who seem to be dying from the virus are actually dying “with COVID-19.” In hard-hit New York State, 86% of the deaths counted have indeed had comorbidities, ranging from diabetes to coronary heart disease.(7) Meanwhile, as of April 24, the median age of a COVID-19 death in Canada is 84.(8) Both of these facts raise the very important question of how many comorbidities or “natural” deaths are being coded incorrectly as COVID-19 deaths in Canada.
This can have a very large effect. Taking Angus’s low range (prevalence of 1%) suggests that 10% of Canada’s COVID-19 deaths could be incidental (see Figure 1). If the true prevalence in Canada is closer to California’s, between 28% and 40% of Canadian COVID-19 deaths could be incidental. And if the true prevalence in Canada is Angus’s higher range of 8%, up to 80% of people apparently dying from the virus in Canada could simply be “dying with” COVID-19.
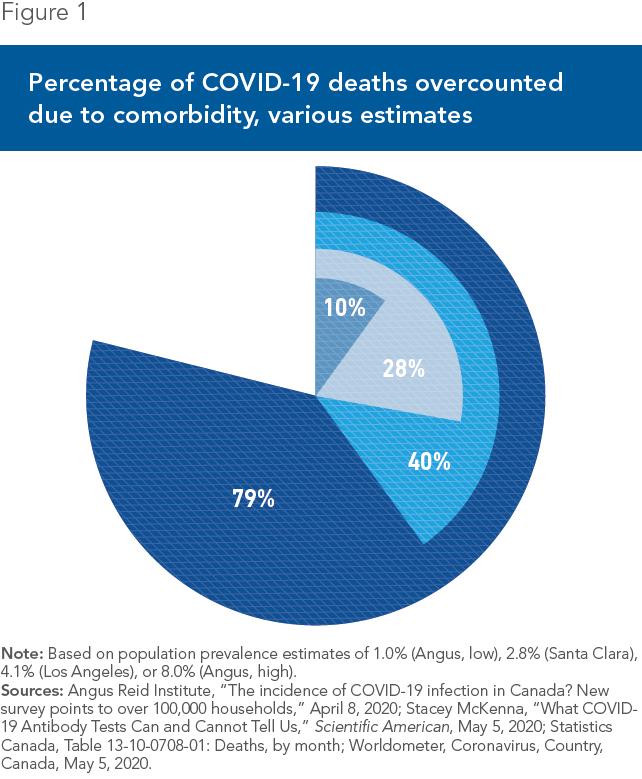
To see why, every month last year, an average of 23,600 Canadians died of other causes.(9) Extrapo-lating, roughly 40,000 Canadians would have died from other causes in the 51 days following Canada’s first COVID-19 death.(10) At a uniform 2.8% prevalence, the lower end in California, statistically 2.8% of those expected 40,000 deaths, so 1,120 people, would have been incidentally infected but would have died anyway. Given actual estimates of 4,000 COVID-19 deaths in Canada, this implies that, statistically, 28% of these deaths could have been “with COVID-19.” At Angus’s higher estimate, this rises to almost 80%.
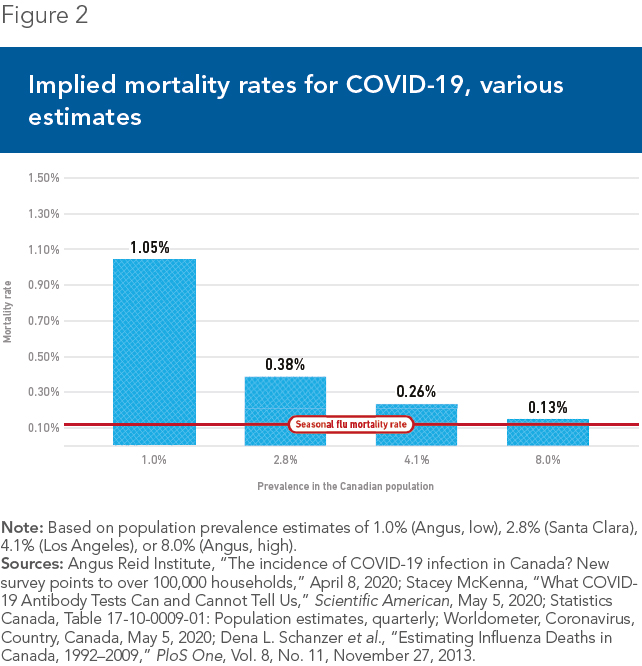
The second important implication is the mortality rate—just how deadly is this virus? A 1% prevalence implies COVID-19 mortality of roughly 1.1%(11)—far lower than early estimates above 3%.(12) If prevalence is at California rates, implied mortality falls further to roughly 0.3%. And if the 8% estimate turns out to be true, implicit mortality would fall to just 0.13%—only slightly higher than the seasonal flu, fatal in 0.11% of cases (see Figure 2).(13)
We Need More Data
We will not know the extent of either effect—the overestimation of deaths and of mortality—until we know population prevalence, especially prevalence by age. And it is possible that delays in death reporting mean we are actually undercounting deaths(14) even if we are overestimating mortality. But if Canada’s prevalence is anything like California’s data and Angus’s survey results, COVID-19 may be killing far fewer Canadians than we think.
While we clearly must remain vigilant, decision-makers should also be aware of the degree to which we are “flying blind” until credible prevalence data exists.
References
- John Lee, “How deadly is the coronavirus? It’s still far from clear,” The Spectator, March 28, 2020.
- Worldometer, Coronavirus, Country, Canada, May 5, 2020.
- Angus Reid Institute, “The incidence of COVID-19 infection in Canada? New survey points to over 100,000 households,” April 8, 2020.
- Stacey McKenna, “What COVID-19 Antibody Tests Can and Cannot Tell Us,” Scientific American, May 5, 2020.
- Worldometer, Coronavirus, Reported Cases and Deaths by Country, Territory, or Conveyance, May 5, 2020.
- Children’s Hospital of Wisconsin, Medical care, Dermatology Program, Conditions, Common skin disorders, Viral Exanthems (Rashes), Chickenpox, 2020.
- Richard Franki, “Comorbidities the rule in New York’s COVID-19 deaths,” The Hospitalist, April 8, 2020.
- Éric Grenier, “How focusing on the age of pandemic victims could blind us to the bigger picture,” CBC News, April 24, 2020.
- Statistics Canada, Table 13-10-0708-01: Deaths, by month.
- Worldometer, op. cit., footnote 2.
- Ibid.
- Financial Times, “‘Utterly unreliable’: The mystery behind the true COVID-19 death rate,” National Post, March 31, 2020.
- Dena L. Schanzer et al., “Estimating Influenza Deaths in Canada, 1992–2009,” PloS One, Vol. 8, No. 11, November 27, 2013.
- Alan Freeman and Samuel Freeman, “Is Canada’s COVID-19 problem much bigger than we think?” iPolitics, April 16, 2020.

